She lost her legs and most of her fingers because she didn’t recognize the signs of sepsis.
by Larry Borowsky
When her youngest daughter headed off to college, Katy Grainger found herself at a crossroads in life. After 20-plus years as a stay-at-home mom, she needed to find new outlets for her talents and energy.
“One of the things I wanted to do was to see if I could get onto a nonprofit board,” Grainger says. “I was asking myself: What am I passionate about?
She got her answer the hard way, via a harrowing health emergency that began one Friday afternoon in 2018. A purple sore on Grainger’s right thumb began to ooze, so she stopped at a clinic for an antibiotic prescription. Within 36 hours she would be fighting for her life.
Grainger’s seemingly minor injury was a harbinger of sepsis, a complication of infection that kills roughly 250,000 Americans a year and causes limb loss in thousands of patients. Like most sepsis victims, Grainger didn’t recognize the symptoms or realize how urgently she needed to act. As her fatigue, body aches, and nausea steadily worsened, she kept trying to sleep it off and ride it out. When she finally texted a friend on Sunday morning to ask for help, it was almost too late.
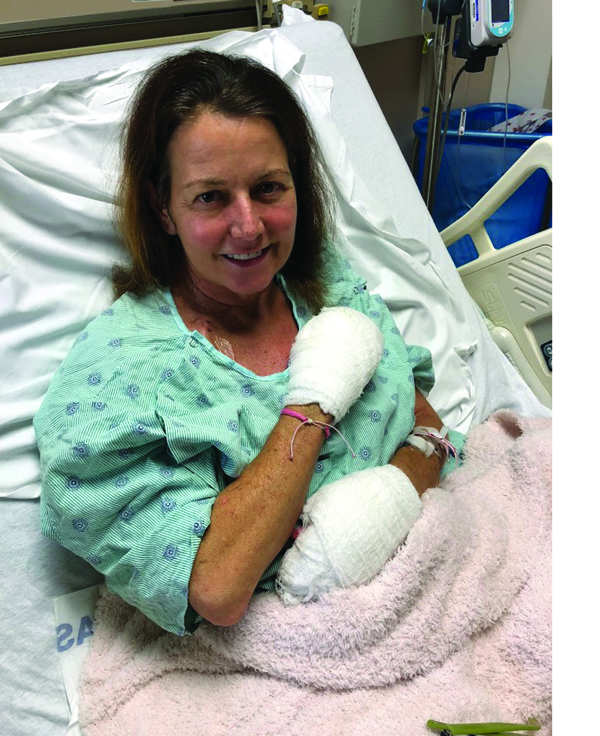
“I went into septic shock at home,” says Grainger. “I barely survived. With every hour you wait, a person has an 8 percent greater chance of dying. I’d used almost all my time by the time I got to the hospital, because I didn’t know the signs and symptoms.”
Doctors placed her in a medically induced coma to give her body a fighting chance. When she emerged a week later, her fingertips and feet had turned almost black. In the end, Grainger lost her legs below the knee, as well as seven fingers. Yet the experience filled her with gratitude to be alive—and set the stage for the next act in her life.
“I was already in this period of transition, trying to figure out my passion,” she says. “And then all of a sudden I got sepsis and came out the other side, and I thought: ‘I’m passionate about this.’”
Time to Make a Difference
Grainger is now one of the nation’s leading advocates for sepsis awareness. She sits on the board of the Sepsis Alliance, a national advocacy organization that supports survivors and educates medical professionals and policy makers. She has shared her story in all kinds of settings, from Congressional hearings to medical conferences, corporate retreats, schools, and national media such as the Today show. A YouTube video about Grainger’s ordeal has drawn more than 200,000 views. In mid-September she’ll be taking part in the three-day Sepsis Summit, one of the key highlights of Sepsis Awareness Month.
“Katy has been an incredible addition to the Sepsis Alliance board of directors,” says Thomas Heymann, the organization’s president and CEO. “We need passionate individuals to help us drive systemic change. Katy has been fearless in using her story in an effort to raise sepsis awareness and save lives and limbs.”
The Centers for Disease Control and Prevention (CDC) estimate there are 1.7 million cases of sepsis every year—twice as many as the number of heart attacks. Yet heart attack warning signs are far more widely recognized than the symptoms of sepsis. Roughly a quarter of American adults have never even heard of the disease, and a third can’t name a single symptom.

“Sepsis is the public health crisis that no one is talking about,” Heymann says. “Despite the millions of lives sepsis impacts and its immense economic toll, the public is much more familiar with conditions, such as stroke and diabetes, which take far fewer lives.”
“Part of the problem is that sepsis is classified as a ‘clinical syndrome’ as opposed to a disease,” adds Grainger. “It’s your body’s reaction to an infection. Your immune system goes haywire, it overreacts, and it starts attacking healthy tissue.”
Even among people who’ve heard of sepsis, confusion abounds. Many Americans mistakenly believe that sepsis only kills infants and elderly patients. Others think sepsis only strikes at the hospital, preying on patients who’ve already been weakened by some other illness. Both perceptions are partly true—sepsis risks are indeed elevated among the very young and very old, and the condition often does hit people who are ill with pneumonia, urinary tract infections, abdominal illness, and other maladies. But sepsis also strikes tens of thousands of people who, like Grainger, are healthy adults in the prime of their lives. Only 20 percent of cases occur in the hospital—the other 80 percent originate at home, work, or elsewhere in the community.
About one in ten cases results in limb loss, and sepsis often has other long-range health implications. “People often experience cognitive issues, memory loss, or chronic fatigue,” says Grainger. “Neuropathy is also common. Even if someone didn’t lose limbs, their limbs may be damaged and they walk around in constant pain.”
The Sepsis Alliance’s “It’s About Time” campaign offers health providers, government officials, and members of the public an easy-to-remember mechanism for recognizing and remembering the signs of sepsis. The organization’s fundraising campaigns, webinars, legislative initiatives, and other programs are helping to create an infrastructure that supports more effective sepsis responses. The Alliance is also working to build a national sepsis registry to track survivors’ short- and long-term outcomes. More comprehensive data would do more than promote public understanding, says Grainger. It would also advance clinical insights to help doctors and nurses better serve their patients.
Getting that data could paint a more precise picture of how many amputations are caused by sepsis. The Amputee Coalition estimates that about 14,000 people a year lose at least one limb to sepsis, but the true figure might be above 20,000. A registry might also answer a question that’s near and dear to Grainger: Why do some healthy people with very small infections end up with sepsis?
“My husband can go around with 87 infected cuts on his body at any given time, and nothing ever happens to him,” she laughs. “They haven’t been able to study this to understand how something as minor as a bump on your thumb, in my case, can have you dying in the hospital a few hours later.”
Kindness Goes a Long Way
Grainger was near death when she arrived at the hospital. When her life was finally out of danger, doctors turned their attention to saving her limbs.
“The tips of my fingers were black, and I knew they were dead,” she says. “I heard my doctors saying the soles of my feet were black, too. I could logically realize that if the soles of my feet are dead, they’re not worth salvaging. But it took me a full three weeks to admit it. No one was allowed to use the word ‘amputation.’ It’s a scary word.”
When she ultimately accepted that amputation was her best course of action, Grainger was fortunate to have a trusted resource she could turn to. Three years earlier, an old family friend got sepsis from strep throat during her sophomore year of college. The young woman ended up losing one leg below the knee and the toes on her other foot.
“That girl was in my house constantly from kindergarten through seventh grade,” Grainger says. “She and my daughter were very best friends, and the families were super close. So when I knew I was going to have my legs amputated, we got on Facetime with her so she could show me her prosthesis. She showed me how easy it is to take on and off, she showed me her residual limb, and that was so helpful. She’s basically been my mentor through this whole process.”
Grainger has paid that favor forward by supporting the limb-loss community at every opportunity. Earlier this year she got certified as an Amputee Coalition Lead Advocate, and she’s planning to get certified as a Peer Mentor as well. She speaks frequently to groups of adults, schoolkids, and other audiences, with the goal of normalizing limb difference and disability.
“Part of my mission is to show people that it’s ok,” she says. “I have nothing to hide. I’m just a normal person. I wear shorts as often as I can. It’s kind of awkward to cover up the prosthetics with pants, so I’d rather just put it out there. I’m someone who didn’t have exposure to people who had amputations or people in wheelchairs before this happened to me. Having conversations about it is a great way to educate people.”
At the same time, Grainger has been pleasantly surprised at how understanding most people are. People open doors for her and commit other small acts of kindness—although they’re not as kind when she’s wearing long pants and they can’t see her prostheses. There’s a lesson in that, Grainger believes.
“Even if you can’t see what’s going on with a person, it doesn’t mean they aren’t struggling with things that are very difficult,” she says. “We all have problems in our life. It could be a health condition, it could be a loss. That’s part of my message: Be nice to everyone, because you don’t know what they’re dealing with.”
SIGNS OF SEPSIS
The Sepsis Alliance’s “It’s About Time” campaign uses the acroynm “T-I-M-E” to educate people about the key warning signs of sepsis. The letters stand for:
T Temperature. Watch for unusually high or low temperatures
I Infection. A virus, superficial wound, or recent surgical procedure can precipitate a septic reaction.
M Mental status. Drowsiness, confusion, and memory loss are common in septic patients.
E Extreme illness. Severe flu-like symptoms, including nausea, pain, and shortness of breath, may indicate sepsis.
“Time” is also significant, of course, because every hour that passes increases the odds that it might claim a limb—or your life. Learn more at sepsis.org.