Meet the researchers who are working to make sockets fit better than ever.
By Jessica Ennis
Innovation has moved prosthetic design from the realm of science fiction into reality. You can readily find artificial limbs that have been 3D printed, can move intuitively with artificial intelligence (AI), or can even “feel” using neurosensors. However, the critical interface that joins the wearer to their prosthesis has been long overdue for a high-tech makeover.

“Socket fit is the number-one most important part of a prosthesis,” says Emily Harvey, who has worn a prosthetic leg since undergoing an amputation at age two. “What we’ve seen so far for investment in this industry is more flashy things like the powered knees and feet. And those things are wonderful, but high tech is useless if you don’t have a good-fitting socket. Even then, you’ll have days that are hard.”
Fortunately, easier days may lie ahead. A handful of engineering teams are answering the call for change by relentlessly pursuing dramatic advancements in socket and liner fit. While these novel solutions are in varying stages of development, they’re getting closer to the finish line.
They can’t get there soon enough for Harvey, who has little time to waste on socket-related disruptions and recovery. She’s a disability rights attorney, the founder of a nonprofit for amputees, an author of three children’s books, and an active outdoor explorer in her home state of Colorado.
Harvey jokes that her decades-long quest to achieve a long-lasting, comfortable socket fit is akin to “The Princess and the Pea” fairy tale: No matter what she layers on or takes away, nothing feels great all the time. “I can feel everything, even a seam on a liner,” she says, adding with a tinge of exasperation: “I’ve pretty much tried it all and ultimately landed back in a gel sock with a Pelite foam liner, just like I first began using when I was two.”
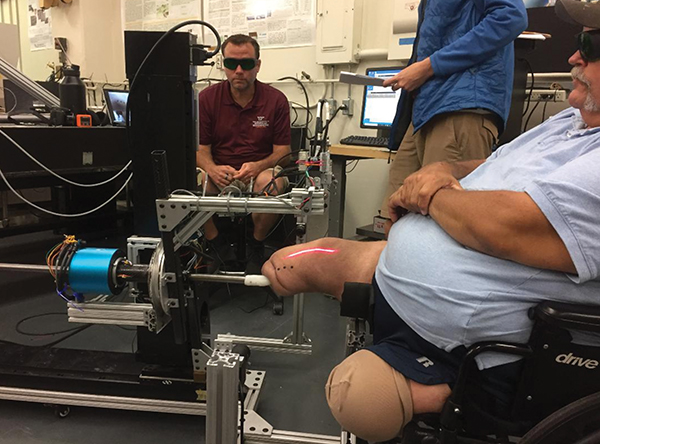
Tech’s smart socket. Courtesy of Virgina Tech.
Lower-limb amputees are all too familiar with the frustrations associated with volume change in their residual limbs and the drastic effect on socket fit and alignment. Despite multiple sock changes and other adjustments throughout the day to add or reduce thickness, pistoning sockets inevitably cause sore spots, blisters, rashes, and other maladies—not to mention more serious problems such as knee, back, and hip problems. Urgent issues such as loss of circulation can force an abrupt removal of the prosthesis, no matter where the wearer is or what they’re doing.
For some, these problems are just too much to handle. A 2019 Agency for Healthcare Research and Quality report estimated that anywhere from 11 percent to 22 percent of lower-limb amputees end up abandoning their prostheses after about a year.
Smarter sockets hold the potential to reduce or eliminate all of these problems. Amplitude took a deeper look at a few of the most promising smart-socket projects to better understand the technology and get a sense of when consumers might see something on the market.
AI-enabled Prosthetic Liner from UNHINDR
Across the pond, the world’s first socket liner that uses AI to adapt and change with the wearer’s residual limb is already making a splash—and it hasn’t even launched yet.
Roliner is the brainchild of Ugur Tanriverdi, co-founder and CEO of the London-based startup Unhindr. Since 2018, Tanriverdi has generated quite the buzz for Roliner, raising approximately $1.65 million in seed funding via investors, grants, and innovation awards. The company is backed by EIT Health, a branch of the European Institute of Innovation and Technology.
“The amputee is at the center of everything we do,” Tanriverdi says. “Our technology adapts to the user’s lifestyle; they don’t have to adapt to the technology.”
The liner works by using AI to read real-time data from small sensors placed outside the prosthetic socket. Roliner learns the wearer’s comfort preferences over time, then continuously adjusts the liner’s fit by filling or emptying microchannels (tubes smaller than 1 millimeter in diameter) with tiny amounts of fluid.
Like other liners on the market, Roliner is made from silicone, can be cut to size, and is washable. It also can be used with any existing socket.
“Our design requirements were that Roliner be small, compact, and lightweight, with a long-lasting battery,” Tanriverdi says. “You can’t do something as big as a minifridge or backpack and expect people to wear it. We knew that there were some adaptive sockets commercially available, but we believe an adaptive liner could deliver more value to amputees.”
A doctoral candidate in bioengineering at the Imperial College of London, Tanriverdi holds master’s degrees in engineering design and medical device design and entrepreneurship. He developed an early prototype of the Roliner in 2016 while working at an advanced systems lab run by Firat Guder, PhD, in Imperial’s Department of Bioengineering.
Guder co-founded Unhindr with Tanriverdi and now serves as the company’s chief scientific officer. The team is rounded out by chief technology officer Guglielmo Senesi, Tarek Asfour serving as product engineer, and vascular surgeon Joseph Shalhoub, who is the clinical investigator.
Although the Roliner isn’t available to consumers yet, it’s making steady progress. Tanriverdi and his team have filed several patents and launched prototype trials at Imperial College. A national clinical trial will begin in the UK in early 2022. Although pricing has not been set yet, Tanriverdi stressed that it’s important to keep Roliner affordable. The company might offer different versions of the Roliner at various price points, and it’s working through the requirements for potential insurance coverage. Keep eyes open for a soft launch sometime next year.
Motor-driven Sockets From the University of Washington
After dedicating more than a quarter of a century to improving the fit of prosthetic devices, University of Washington bioengineering professor Joan Sanders and her team have moved into the realm of smart sockets.
Their auto-adjusting socket aims to let prosthesis users wear their devices without pain or distraction during high-intensity use. The team designed, implemented, and tested a control system that automatically maintains socket fit by continuously adjusting the socket size.
“Our auto-adjusting socket enables hands-free, immediate socket-fit changes,” says Kate Allyn, a past president of the American Academy of Orthotists and Prosthetists and the research prosthetist in Sanders’ lab for the past 14 years. “These auto adjustments are small, [frequent], and undetectable to the user until they realize their socket is more comfortable over the day. This technology will be invaluable to people who may not have keen sensation on their residual limb. The clinical impact for this technology is incomparable.”
Focusing on individuals with transtibial amputations, the team developed the automatic system by creating adjustable sockets for 12 participants and investigating how limb fluid volume changed when socket size changed.
The sockets contain motor-driven adjustable panels fastened to mounts within the socket wall. A microcontroller commands the motors to move in or out slightly, and it keeps a running log of panel positions to track socket volume changes over time. Sanders’ team built custom sensors into the socket, and these prompt the control system to adjust whenever changes in fit are detected.
Participants tested the system by walking on a treadmill to determine if the socket could maintain a target and respond accurately to changes. In a paper published in December 2020, Sanders and her colleagues concluded the system worked and was ready for evaluation outside the lab. The project has since moved into clinical trials, with 12 participants wearing the socket at home for several weeks.
In a separate project, being conducted in collaboration with the Army’s Center for the Intrepid, the UW team is testing its smart-socket technology under military conditions. That research is being funded by a $1.5 million Department of Defense grant. Testing on the study’s first participant was completed late this summer.
“The innovation we are working on now will benefit prosthesis users in their daily life, no matter how active they are,” Allyn says. “Physical activity has a huge impact on quality of life, and we aim to improve prosthetic care using our technology.”
Sanders and the UW team are developing a second socket-improvement technology called a release-relock socket. This innovation allows the wearer to release socket pressure while sitting, yet never lose contact with their prosthesis. With the push of a button, the socket can be donned, partially donned, or doffed. Pilot testing has concluded, clinical trials are underway, and there’s already a second generation of the technology in development.
Smart Materials Make a Smart Socket at Virginia Tech
In 2008, Virginia Tech researcher Michael Philen approached his colleague Michael Madigan with an idea.
Philen, an associate professor of Aerospace and Ocean Engineering, believed the smart materials he had been working with to help develop morphing airplane wings could be used to create a smart socket that would accommodate volume fluctuations in a residual limb. Called flexible fluidic matrix composites, the materials wrap a long rubber tube in a weave of carbon fibers—like a finger trap toy—that can change in volume and stiffness as the tube is pressurized.
Madigan, a biomechanics expert, agreed Philen was onto something and immediately signed on. But it took 11 rejected grant submissions over a decade before their research project finally secured funding in 2019 from the National Science Foundation. “Getting this grant so we could make progress on the idea has really been an exercise in persistence,” Madigan says.
In Madigan and Philen’s prototype socket, flexible fluidic matrix composites are fabricated into thin hockey-puck shapes that correspond to the areas on the residual limb that experience volume change. A small pump injects pressurized fluid into the puck, adjusting its thickness at the precise location of volume change. They designed the system with valuable input from Trevor LeMaster, a congenital above-knee amputee who earned his mechanical engineering degree at Virginia Tech.
“I had a lot of problems with the volume loss of my limb, especially playing middle- and high-school sports,” LeMaster says. “Sometimes I couldn’t fit into my socket; other times I had to wear multiple socks for it to fit. There were times my socket would be so tight that I had to wrap it overnight to decrease its volume or rub Vaseline on my leg to get it on in the morning.”
LeMaster, who is currently pursuing a master’s degree in prosthetics and orthotics at Baylor University, is excited about the progress. “This is a real problem in the field that needs to be solved,” he says. “It would best be accomplished through a socket interface device that is easily adjustable and effective, and I believe the solution the Virginia Tech team developed has the potential to really make an impact on amputees’ lives.”
It may be a while before the team’s smart socket is ready for consumers, though. “Long term, we want socket adjustments to be an automated process where the user doesn’t have to recognize and manually respond,” Madigan says. “We think that is years away, and beyond what we are funded for now. But we are taking steps toward that goal. The technology developed for the manual version works.”
To help move these efforts forward, the team brought on Brian Kaluf, the director of clinical outcomes and research at Ability Prosthetics and Orthotics, as their clinical collaborator. In addition to lending his expertise, Kaluf helps recruit patients to participate in research and testing at Ability’s ten locations across multiple states. A prototype of the smart socket is expected next year, and the team anticipates participants will begin testing it sometime in 2023.
Whenever smart sockets reach the marketplace, amputees such as Emily Harvey will be fired up to give them a try. “I’m eagerly awaiting technological advancements to socket fit,” she says. “If the industry could find a way to consistently improve outcomes in this area, it has the potential to benefit so many of us who just want to go about living our lives without having to stress about how our prosthesis fits on any given day.”




