“One of the biggest problems with prosthetic research is that it’s almost impossible to find data,” says Jefferson Rajah. “And whatever data we have is usually quite bad.”
While there are multiple initiatives afoot to build a robust base of information about amputees (e.g. the National Limb Loss and Preservation Registry), it will take years for those efforts to yield meaningful interpretations. In the interim, Rajah is attempting to glean actionable insights from existing data, using a complex modeling approach called system dynamics.
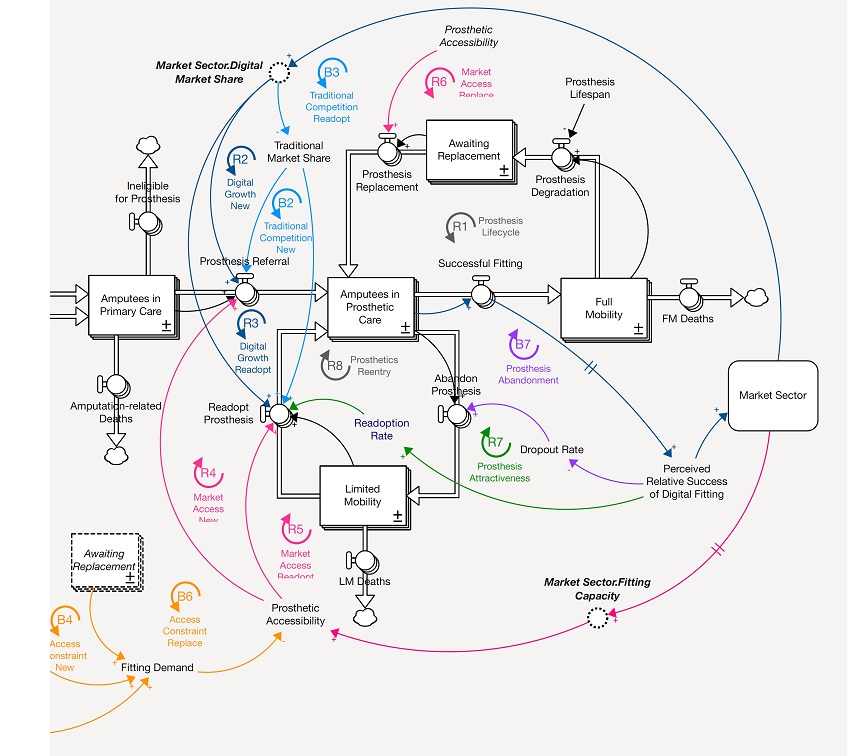
He presented his first study last month at the International System Dynamics Conference in Frankfurt, Germany. Titled “The Dynamics of Prosthetics Care Continuum for Persons With Amputation,” Rajah’s project attempts to identify ways to lower the cost of prosthetic care, remove barriers to access, and get better outcomes for more people.
Here’s one preliminary conclusion: The future of prosthetic sockets is digital. As the socket-fitting process migrates from traditional plaster-casting to digital scanning and 3D-printing, amputees should reap tremendous gains in prosthesis comfort, functionality, and success rates.
“Right now, digital only makes up about 1 percent of the marketplace,” explains Rajah, a graduate student at the University of Bergen, one of the world’s leading centers for system dynamics. “In an optimistic scenario, where digital’s market share grows to 60 percent by 2050, we can expect a doubling of mobility among people with amputation, with significant increases in overall health and economic indicators. Even in our most pessimistic scenario, where digital’s market share only gets to 10 percent, we still see an increase in the mobility rate and in the percentage of people with access to a prosthesis.”
Two evidence-based assumptions underpin Rajah’s analysis. First, it takes less time and money to produce a socket using digital scans than via conventional methods. And second, sockets produced from digital scans tend to be better-fitting than sockets produced from plaster casts. Both factors allow clinicians to create more functionality, per unit of time, than they can at present.
A relatively young discipline, system dynamics grew out of the MIT School of Management in the 1950s and was adopted by General Electric as a decision-making framework. Over time it has migrated from the business environment to other domains involving complex social systems, including health care, education, politics, land development, global trade, technological research, and military engagement.
“In system dynamics, we’re building a model that reflects the interconnections between different variables,” Rajah says. “Then we run different scenarios to analyze how to get the best results, so we can model for uncertainty. Even without complete data, we can identify the leverage points in the system and determine what changes in policy or practice have the most impact.”
In his model for the prosthetic care system, Rajah can twiddle the dials on all sorts of factors. What happens if we pour more money into treatment and prevention programs for diabetes and peripheral artery disease? Suppose we train more prosthetists? rewrite the insurance codes? modify K-level criteria? pour more money into patient education? intensify services and support for low-mobility amputees? The model also includes a free-market component, with nodes that account for R&D investment, entrepreneurial innovation, consumer perceptions, and competition from other technologies.
Although he’s a newcomer to the field of prosthetics, Rajah is drawing on the expertise of some high-powered collaborators. His academic advisor, Paulo Gonçalves, has been working to expand global access to prosthetic devices for more than a decade. A former entrepreneur, he co-founded a humanitiarian company called SwissLeg that provided low-cost prosthetic limbs to civilian victims of warfare in the Middle East, Africa, and Asia. Another collaborator, Christopher Hutchins, is a bilateral amputee and certified prosthetist who co-founded ProsFit, one of Europe’s leading innovators in digital socket manufacturing. And the research is supported by the Toyota Mobility Foundation, whose global mission includes the development of distributed care networks that reduce cost, eliminate bottlenecks, and expand access to prosthetic devices.
“This model is still quite preliminary,” Rajah cautions. “There are parts of the system we’re not actually capturing. So it needs more work. There are ways you can extend this to identify other leverage points. This could be a base model that spurs more work on how to improve amputee care.”




